Services
Medical Billing & Coding Services
We provide reliable medical billing and coding services to help healthcare providers manage their claims efficiently and maintain
accurate documentation. Our team focuses on proper coding and timely submission to support a smoother reimbursement process.
WHY CHOOSE US
Trusted Medical Billing Solutions That Help Your Practice Run Smoother and Get Paid Faster
We provide dependable medical billing and coding support to help healthcare providers manage their claims more efficiently. Our focus is on accurate documentation, proper coding, and timely submissions to support a smoother billing workflow. We work with practices of different sizes and specialties, assisting with common billing challenges such as claim delays, denials, and administrative workload. Our goal is to help you maintain organized billing processes and improve overall efficiency.
- Support accurate claim submission and reduce common errors
- Help improve cash flow with consistent billing processes
- Identify and resolve issues that may delay reimbursements
- Reduce administrative workload for your staff
- Assist with maintaining compliance and proper documentation
- Improve visibility into your billing and revenue cycle
- Help manage and follow up on outstanding claims
- Provide structured support without disrupting your workflow

Integrated Medical Coding for
Clean and Consistent Billing
Within our billing workflow, medical coding plays an important role in preparing claims for submission. We carefully assign CPT and ICD-10 codes based on clinical documentation, helping maintain consistency and supporting a more efficient billing process.
Our approach focuses on reviewing documentation accurately and aligning codes with payer requirements. This helps reduce common errors, improves clarity in claim submission, and supports smoother communication between providers and insurance payers.

How Our Billing Process Works
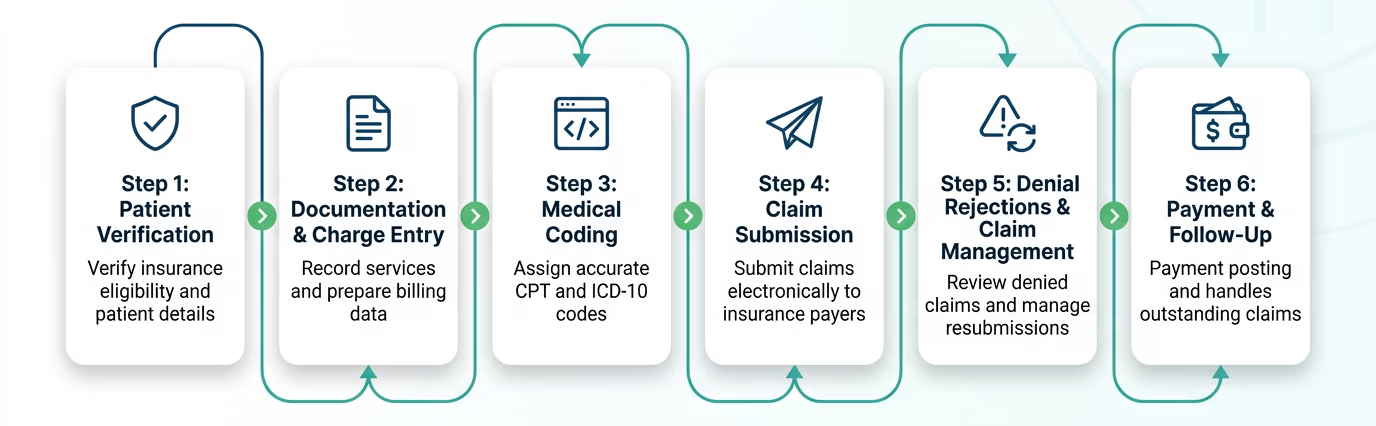

Billing & Coding Audit Services
We provide billing and coding audit services to help healthcare providers review their current processes and identify areas that may need improvement. Our focus is on checking accuracy, documentation alignment, and coding consistency to support a more organized billing workflow.
Our audit process involves reviewing claims, coding practices, and documentation to highlight common issues that may affect billing performance. This includes identifying errors, inconsistencies, or gaps that could lead to delays or denials.
By analyzing existing workflows, we aim to provide clear insights that help practices improve accuracy and maintain better control over their billing operations. Our approach is structured and supportive, allowing providers to understand their current position and make informed improvements where needed.
- Review of coding accuracy and documentation alignment
- Identification of common billing and claim errors
- Analysis of claim submission patterns and workflows
- Support in improving overall billing consistency
- Insights to help reduce avoidable delays or rejections

Physician Credentialing Services to Support
Your Practice Growth
We provide physician credentialing services to help healthcare providers complete the enrollment process with insurance payers in a structured and organized manner. Our focus is on preparing, submitting, and managing credentialing applications to support timely approvals and reduce administrative challenges.
Our credentialing services are built to support different types of healthcare practices, including physicians and multispecialty clinics, with solutions that include:

Medicare, Medicaid,
& Commercial Payer Enrollment
Supporting provider setup with
major insurance networks

Organized Credentialing
Process
Structured preparation and
submission of applications

Accurate Provider
Information Management
Maintaining updated and consistent
provider details

Real-Time Status Tracking
Monitoring progress and keeping
you informed
Ongoing Follow-Up with
Payers
Handling communication and
responding to requests
24/7 Support Availability
Assistance when you need it
during the process